Last updated on March 11th, 2020 at 01:54 am
Adderall is a mixture of amphetamines used to treat ADHD. It works well, but not without some serious side effects. There are many alternatives to adderall that provide similar benefits, but without the side effects. The best nootropics for ADHD improve focus, concentration, and attention while not causing any serious side effects.
These adderall alternatives all work via different mechanisms and in theory can all be combined to produce a synergistic effect, with the exception of ginseng. However, caution should be taken when combining them as too much dopaminergic activity can result in not only the worsening of ADHD symptoms but potentially psychosis.
Many of these nootropics have been proven to be effective for treating ADHD. Some have numerous studies demonstrating a significant effect in ADHD patients. Others, like phenylpiracetam and bromantane, are just hypothesized to help ADHD, but nonetheless have many positive anecdotes.
Summary
| Nootropic | Mechanism of action | Taken | Dosage |
|---|---|---|---|
| Modafinil | Inhibits dopamine reuptake | Either acutely or chronically. Studies found no tolerance | 100 mg to 400 mg |
| Fasoracetam | Modulates glutamate activity | Chronically - Benefits increase the longer it's taken | 50 mg twice a day |
| Bromantane | Increases dopamine production | Chronically - Benefits build up over time | 50 mg to 100 mg |
| Selegiline | Inhibits MAO-B preventing some dopamine breakdown | Chronically - Dopamine accumulates after a few weeks of treatment | 5 mg sublingually |
| Phenylpiracetam | Upregulates dopamine receptors and may act like a stimulant | Either acutely or chronically. Tolerance may form after chronic dosing. | 100 mg to 200 mg |
| Memantine |
| Chronically - Needs to build up. Initial effects may be negative. | 20 mg a day |
| Ginseng | Modulation of dopamine and noradrenaline | Chronically - Research uses chronic dosing | 1000 mg twice a day |
| Iron |
| Chronically - Iron needs time to build up in the system | N/A - Consult your doctor for proper dosing |
| Meditation | Changes in brain structure | Chronically | N/A |
Modafinil
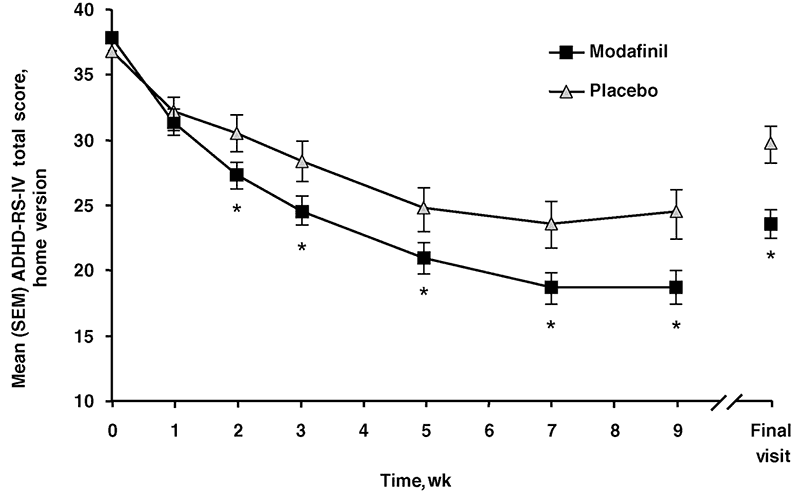
A drug used to treat narcolepsy, modafinil increases dopamine in the brain with almost the same potency as methylphenidate in humans. Several clinical trials have been performed to test the efficacy of modafinil in children, adolescents, and adults with ADHD.[1][2][3][4][5][6] In all these studies, it was shown to significantly reduce symptoms and was well-tolerated.
In comparison to adderall, a study found no withdrawal effects upon discontinuation of modafinil following 2 weeks of treatment in children and adolescents with ADHD.[4]
Interestingly, there were no rebound ADHD symptoms suggesting it may have a long-term benefit. Moreover, a study found modafinil to be equivalent to dextroamphetamine in reducing the symptoms of ADHD – Adderall is a mixture of amphetamine salts that’s 75% dextroamphetamine and 25% levoamphetamine.[5] Regarding dosing, one study found once a day administration to be superior to divided doses.[6]
Fasoracetam
A nootropic drug of the racetam family, fasoracetam is unique in that it doesn’t act a stimulant. In contrast to typical stimulants, it doesn’t seem to increase dopamine and noradrenaline levels. Instead, it acts via glutamate.
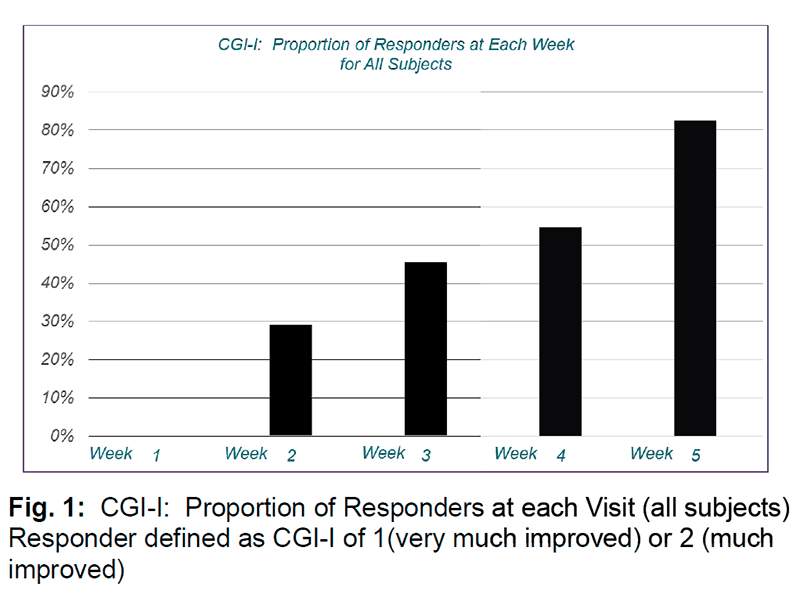
Some ADHD patients have abnormal genes for the glutamate receptors which is thought to cause their symptoms. In a study, adolescents with ADHD and an abnormal glutamate gene were started at 50 mg twice a day and had their dose increased weekly up to a maximum of 500 mg 2x per day.[7]
With each passing week the benefits increased. Side effects were not nearly as harsh compared to adderall. They mainly consisted of headache and fatigue. Plus, since it acts via a different mechanism it can be combined with other nootropics for ADHD, like modafinil. This will result in a synergistic effect.
Bromantane
Also known as ladasten. A very unique compound, bromantane is thought to work by upregulating dopamine production. Tyrosine hydroxylase (TH) is the rate-limiting enzyme that controls L-DOPA production. Aromatic L-amino acid decarboxylase (AAAD), also known as DOPA decarboxylase, is the rate-limiting enzyme that converts L-DOPA to dopamine. The more tyrosine hydroxylase is expressed, the more L-DOPA is produced. Likewise, the more AAAD is expressed, the more dopamine is produced.
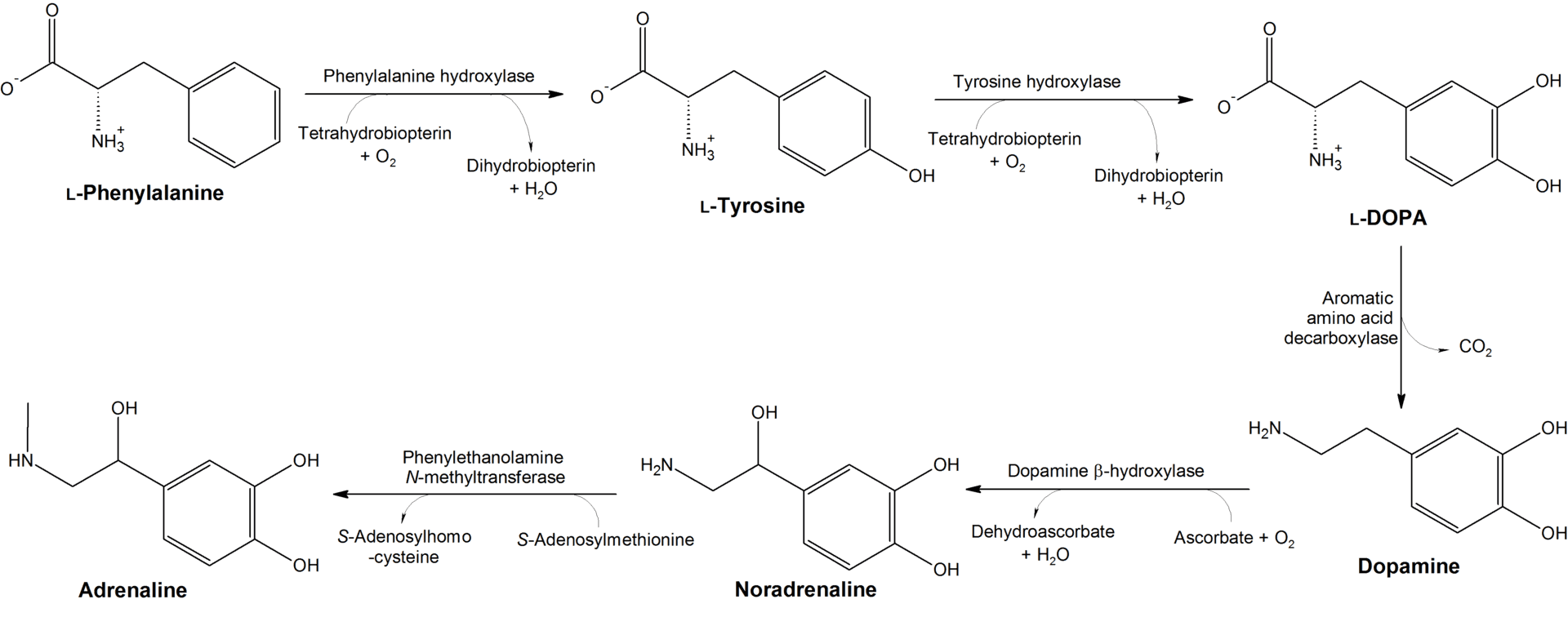
Bromantane was shown to remarkably enhance the expression of both tyrosine hydroxylase and AAAD in rats, and the effects were rapid and long-lasting. [8][9][10] Moreover, it seems bromantane also increases dopamine release in the striatum of rats and it has been noted to last up to 8 hours.[11]
As few studies have been on humans, caution should be taken for those already sensitive to dopaminergics. It is not yet known if the effects of bromantane are permanent or semi-permanent. In rats, it definitely seems to last a long time.
Selegiline
Commonly known as Deprenyl or EMSAM, selegiline is a classic nootropic that has been shown to possess remarkable benefits. It enhances memory and learning, mood, libido, motivation, focus, and may even extend lifespan in humans. It was already shown to extend the lifespan of rats.
Selegiline works by binding to an enzyme known as MAO-B, short for monoamine oxidase type B. This is one of the main enzymes to breakdown or metabolize dopamine and phenethylamine (PEA). PEA is an endogenous compound that releases dopamine and noradrenaline.
In fact, amphetamines like adderall are derived from PEA. The brain continuously produces PEA, but because of MAO-B it has a very short half-life of just 10 minutes. When MAO-B is eliminated, however, the half-life becomes much longer.
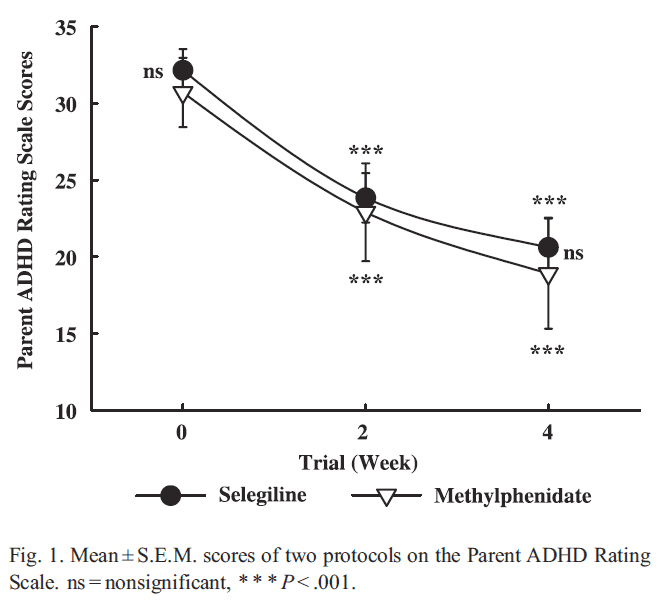
So not only does selegiline increased dopamine levels, but it also increases PEA levels which in turn increases dopamine release. Several studies have shown selegiline to improve ADHD symptoms on its own, and with one study finding it comparable to methylphenidate, but with much fewer side effects.[12][13][14]
Though, a study found it ineffective in treating impulsivity, but nonetheless found it effective for the inattentive type of ADHD.[15]
Phenylpiracetam
 Also known as phenotropil. A nootropic of the racetam family, phenylpiracetam has been shown to upregulate several dopamine receptors involved in ADHD and focus.[16] In addition, it seems to have a stimulant-like effect with many anecdotes supporting this notion.[17]
Also known as phenotropil. A nootropic of the racetam family, phenylpiracetam has been shown to upregulate several dopamine receptors involved in ADHD and focus.[16] In addition, it seems to have a stimulant-like effect with many anecdotes supporting this notion.[17]
Phenylpiracetam is unique in this list in that it has both acute and chronic effects, the acute being the stimulant-like effect and the chronic being the upregulation of the dopamine receptors. However, not much research has been done on this nootropic and many users find its effects begin to wane the longer they take it.
Indeed, there is some Russian research to support this claim where after 4-8 weeks of treatment, the effects of phenotropil were decreased as compared to the first few weeks.[18]
Memantine
Though not designed to treat ADHD, memantine has found a new use within the ADHD and nootropic community. In light of its ability to prevent opiate tolerance, some users have speculated that it may also prevent stimulant tolerance. Moreover, it also appears to enhance some of the positive effects of stimulants; in a study on humans, memantine administered for 7-10 days prior to cocaine consumption was able to enhance cocaine’s subjective high feelings and overall positive effects.[19]
Regardless, not many studies have been done to assess its effects on stimulant tolerance.
However, memantine alone has been found to be effective for ADHD. In one study, 34 adults aged 18-55 were titrated on a dose of 10 mg twice a day. After 6 weeks, there were significant improvements in attention, working memory, and other executive domains.[20] In another study, children aged 6-12 years were given memantine for 8 weeks and improvements in ADHD symptoms were noted. However, those receiving 20 mg had larger improvements and were more likely to complete the trial than those receiving 10 mg.[21]
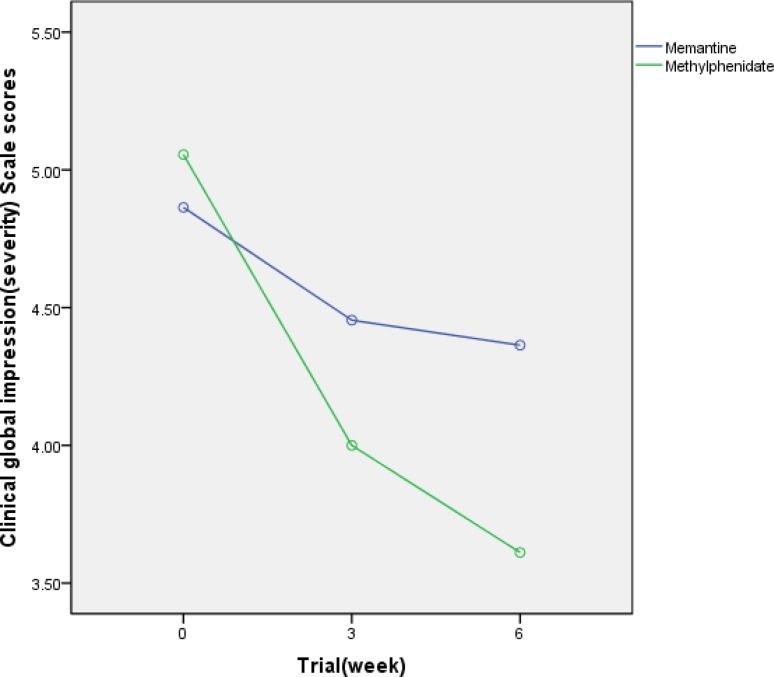
Compared to stimulants for ADHD, memantine was found to be less effective than methylphenidate in reducing ADHD symptoms in children and adolescents.[22] On the other hand, a small study found that memantine and extended-release methylphenidate combined well to produce a synergistic effect.[23]
Ginseng
 Ginseng seems to be a wonder herb that miraculously offers many health benefits, but a lot of these claims have yet to be confirmed by research. Luckily, one of them has been, and that is ginseng’s effect on ADHD. It has long been touted that ginseng can improve focus, energy, and improve overall cognitive function, and recent research backs these claims up.
Ginseng seems to be a wonder herb that miraculously offers many health benefits, but a lot of these claims have yet to be confirmed by research. Luckily, one of them has been, and that is ginseng’s effect on ADHD. It has long been touted that ginseng can improve focus, energy, and improve overall cognitive function, and recent research backs these claims up.
In one study, children aged 5-16 years old received either ginseng or placebo twice a day. At the 8 week mark there were significant improvements in inattention and hyperactivity with the authors concluding that ginseng may be a viable treatment option for ADHD.[24] Another study also found improvements in hyperactivity, inattention, and immaturity in 3 teenagers aged 14-17.[25] Finally, one case study involving a 7 year old boy found 1800 mg of ginseng a day for 8 weeks improved his symptoms of ADHD and several ADHD rating scales.[26]
The mechanism of Ginseng is not yet fully known, but it’s believed to increase dopamine and noradrenaline activity.[27] However, at the same time it may also modulate it. What this means is that ginseng on its own can normalize levels of dopamine and noradrenaline in the brain.
But, combining ginseng with other substances that increase dopamine, like adderall, will antagonize or blunt their effects. There are lots of studies in animals where ginseng inhibited dopamine release caused by stimulants such as cocaine, nicotine and even methamphetamine.[28][29][30][31]
Iron
Iron is well-known to be essential for a variety of different functions in the body. Iron deficiency results in low energy, general weakness, but also a condition known as restless leg syndrome (RLS). This syndrome is directly linked to dopamine dysfunction.[32] In other words, low iron results in low dopamine.
Indeed, when we look at the production steps of dopamine we can see that iron is required for converting Phenylalanine into Tyrosine and Tyrosine into L-DOPA. However, iron goes beyond this and is very important in maintaining normal dopamine receptor function.[33][34][35]
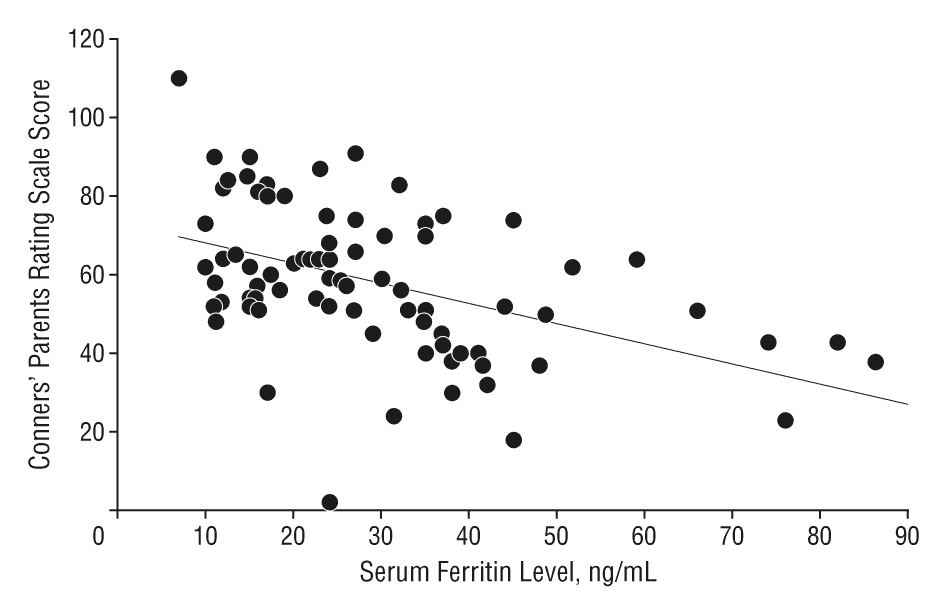
In fact, there are many studies in which iron was found to be effective at treating ADHD symptoms, particularly in those with low ferritin levels.[36] Ferritin is a protein that binds to iron and transports it in the bloodstream or serum. There appears to be an inverse relationship between serum ferritin levels and ADHD symptoms, i.e. the lower the iron levels are the more severe the ADHD symptoms and vice-versa.
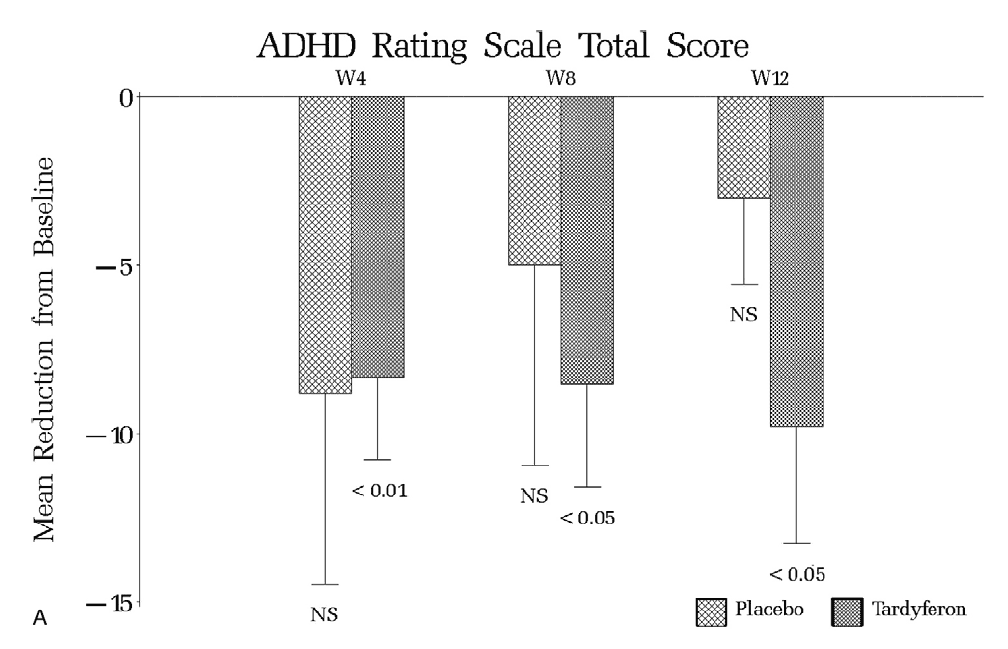
One study utilizing 14 boys aged 7-11 years old found iron supplementation to raise serum ferritin levels and subsequently decrease ADHD scores from 17.6 ± 4.5 to 12.7 ± 5.4.[37] Another study involving children aged 5-8 years old with serum ferritin levels less than 30 ng/mL found a progressive decrease in ADHD scores during the 12 weeks of treatment.[38] The authors of this study also concluded that iron supplementation was as effective as stimulants in treating ADHD.
Warning: Iron supplementation can be dangerous as the body has no way to discard or remove excess iron. Prolonged supplementation, especially with high doses, should be done under a doctor’s supervision with regular bloodwork done to assess iron levels in the body.
Meditation
 While not something you can ingest, more and more evidence has come forth revealing the beneficial effects of meditation on the brain. Meditation changes the brain structure and improves many cognitive factors including attention. There are many ways to meditate and one method that’s widely used in research is called mindfulness meditation.
While not something you can ingest, more and more evidence has come forth revealing the beneficial effects of meditation on the brain. Meditation changes the brain structure and improves many cognitive factors including attention. There are many ways to meditate and one method that’s widely used in research is called mindfulness meditation.
In essence, this technique is simply focusing on being in the present, i.e. being aware of where we are, what we’re doing, and to ignore what’s going on around us. Of course, being able to do this requires tremendous effort. However, you have to think of it as a game and you’re starting at level 1. At first it will feel impossible, but the more you do it, the easier it becomes.
Now, on to the science. In a study involving 24 adults and 8 adolescents with ADHD, 8 weeks of mindfulness meditation resulted in self-reported improvements in not only their ADHD symptoms, but also anxiety and depression.[39] A similar 8-week study with 11 adults with ADHD also found improvements in both self-reported ADHD symptoms and clinician ratings of ADHD.[40]
Mindfulness is not the only method that offers benefits to those with ADHD. Transcendental Meditation (TM) was also found to significantly reduce the symptoms of ADHD in 2 separate studies, with one of the studies finding that TM also resulted in increased verbal fluency.[41][42]
References
- Greenhill, Laurence L. et al. “A Randomized, Double-Blind, Placebo-Controlled Study of Modafinil Film-Coated Tablets in Children and Adolescents With Attention-Deficit/Hyperactivity Disorder.” Journal of the American Academy of Child &Amp; Adolescent Psychiatry, PAP, 2006, doi:10.1097/01.chi.0000205709.63571.
- Biederman, J. et al. “Efficacy and Safety of Modafinil Film-Coated Tablets in Children and Adolescents With Attention-Deficit/Hyperactivity Disorder: Results of a Randomized, Double-Blind, Placebo-Controlled, Flexible-Dose Study.” Pediatrics, vol. 116, no. 6, Jan. 2005, doi:10.1542/peds.2005-0617.
- Kahbazi, Manijeh et al. “A Randomized, Double-Blind and Placebo-Controlled Trial of Modafinil in Children and Adolescents with Attention Deficit and Hyperactivity Disorder.” Psychiatry Research, vol. 168, no. 3, 2009, pp. 234–237. doi:10.1016/j.psychres.2008.06.024.
- Swanson, James M. et al. “Modafinil Film-Coated Tablets in Children and Adolescents With Attention-Deficit/Hyperactivity Disorder: Results of a Randomized, Double-Blind, Placebo-Controlled, Fixed-Dose Study Followed by Abrupt Discontinuation.” J. Clin. Psychiatry The Journal of Clinical Psychiatry, vol. 67, no. 01, 2006, pp. 137–147. doi:10.4088/jcp.v67n0120.
- Taylor, Fletcher B., and Joan Russo. “Efficacy of Modafinil Compared to Dextroamphetamine for the Treatment of Attention Deficit Hyperactivity Disorder in Adults.” Journal of Child and Adolescent Psychopharmacology, vol. 10, no. 4, 2000, pp. 311–320. doi:10.1089/cap.2000.10.311.
- Biederman, Joseph et al. “A Comparison of Once-Daily and Divided Doses of Modafinil in Children with Attention-Deficit/Hyperactivity Disorder: a Randomized, Double-Blind, and Placebo-Controlled Study.” J. Clin. Psychiatry The Journal of Clinical Psychiatry, vol. 67, no. 05, 2006, pp. 727–735. doi:10.4088/jcp.v67n0506.
- Jones, Grace. “Exploratory dose-escalation study of NFC-1 in ADHD adolescents with glutamatergic gene network variants.” 62nd Annual Meeting. AACAP, 2015.
- Mikhaylova, M., et al. “The effects of ladasten on dopaminergic neurotransmission and hippocampal synaptic plasticity in rats.” Neuropharmacology 53.5 (2007): 601-608.
- Vakhitova, IuV, R. S. Iamidanov, and S. B. Seredinin. “Ladasten induces the expression of genes regulating dopamine biosynthesis in various structures of rat brain.” Eksperimental’naia i klinicheskaia farmakologiia 67.4 (2003): 7-11.
- Zimin, I. A., et al. “Role of the brain dopaminergic and serotoninergic systems in psychopharmacological effects of ladasten and sydnocarb.” Eksperimental’naia i klinicheskaia farmakologiia 73.2 (2010): 2-5.
- Grekhova, T. V., et al. “Effect of bromantane, a new immunostimulating agent with psychostimulating activity, on the release and metabolism of dopamine in the striatum of freely moving rats. A microdialysis study.” Bulletin of Experimental Biology and Medicine 119.3 (1995): 294-296.
- Mohammadi, Mohammad Reza, et al. “Selegiline in comparison with methylphenidate in attention deficit hyperactivity disorder children and adolescents in a double-blind, randomized clinical trial.” Journal of Child & Adolescent Psychopharmacology 14.3 (2004): 418-425.
- Akhondzadeh, Shahin, et al. “Selegiline in the treatment of attention deficit hyperactivity disorder in children: a double blind and randomized trial.” Progress in Neuro-Psychopharmacology and Biological Psychiatry 27.5 (2003): 841-845.
- Feigin, A., et al. “A controlled trial of deprenyl in children with Tourette’s syndrome and attention deficit hyperactivity disorder.” Neurology 46.4 (1996): 965-968.
- Rubinstein, Suzanne, et al. “Placebo-controlled study examining effects of selegiline in children with attention-deficit/hyperactivity disorder.” Journal of Child & Adolescent Psychopharmacology 16.4 (2006): 404-415.
- Firstova, Yu Yu, et al. “The effects of scopolamine and the nootropic drug phenotropil on rat brain neurotransmitter receptors during testing of the conditioned passive avoidance task.” Neurochemical Journal 5.2 (2011): 115-125.
- “Phenylpiracetam – Review of Benefits, How It Works, Side Effects, Dosage.” NeuroNootropic. NeuroNootropic, 08 Nov. 2016.
- Medvedev, V. E., V. I. Frolova, and A. V. Epifanov. “New possibilities of pharmacotherapy in cardiovascular patients with mental disorders.” Zhurnal nevrologii i psikhiatrii imeni SS Korsakova 114.9 (2013): 30-37.
- Collins, Eric D., et al. “The effects of memantine on the subjective, reinforcing and cardiovascular effects of cocaine in humans.” Behavioural pharmacology 9.7 (1998): 587-598.
- Surman, Craig BH, et al. “A pilot open label prospective study of memantine monotherapy in adults with ADHD.” The World Journal of Biological Psychiatry 14.4 (2013): 291-298.
- Findling, Robert L., et al. “A pilot evaluation of the safety, tolerability, pharmacokinetics, and effectiveness of memantine in pediatric patients with attention-deficit/hyperactivity disorder combined type.” Journal of child and adolescent psychopharmacology 17.1 (2007): 19-33.
- Mohammadi, Mohammad Reza, Soleiman Mohammadzadeh, and Shahin Akhondzadeh. “Memantine versus methylphenidate in children and adolescents with attention deficit hyperactivity disorder: a double-blind, randomized clinical trial.” Iranian journal of psychiatry 10.2 (2015): 106.
- Biederman, Joseph, et al. “Memantine in the Treatment of Executive Function Deficits in Adults With ADHD A Pilot-Randomized Double-Blind Controlled Clinical Trial.” Journal of attention disorders (2014): 1087054714538656.
- Ko, Hae-Jin, et al. “Effects of Korean red ginseng extract on behavior in children with symptoms of inattention and hyperactivity/impulsivity: a double-blind randomized placebo-controlled trial.” Journal of child and adolescent psychopharmacology 24.9 (2014): 501-508.
- Niederhofer, H. “Panax ginseng may improve some symptoms of attention-deficit hyperactivity disorder.” Journal of dietary supplements 6.1 (2009): 22-27.
- Yuk, Keun Jeong, et al. “Panax Ginseng Extract in a Boy with Attention Deficit Hyperactivity Disorder.” Korean Journal of Psychopharmacology 21.1 (2010): 35-39.
- Kim, Young Choong, et al. “Effect of the saponin fraction of Panax ginseng on catecholamines in mouse brain.” Archives of Pharmacal Research 8.1 (1985): 45-48.
- Shim, In-Sop, et al. “Modulatory effect of ginseng total saponin on dopamine release and tyrosine hydroxylase gene expression induced by nicotine in the rat.” Journal of ethnopharmacology 70.2 (2000): 161-169.
- Kim, Hack-Seang, and Kil-Soon Kim. “Inhibitory effects of ginseng total saponin on nicotine-induced hyperactivity, reverse tolerance and dopamine receptor supersensitivity.” Behavioural brain research 103.1 (1999): 55-61.
- Kim, Hack-Seang, et al. “Blockade by ginseng total saponin of the development of methamphetamine reverse tolerance and dopamine receptor supersensitivity in mice.” Planta medica 61.01 (1995): 22-25.
- Lee, BomBi, et al. “Inhibitory effects of ginseng total saponins on behavioral sensitization and dopamine release induced by cocaine.” Biological and Pharmaceutical Bulletin 31.3 (2008): 436-441.
- Allen, Richard. “Dopamine and iron in the pathophysiology of restless legs syndrome (RLS).” Sleep medicine 5.4 (2004): 385-391.
- Youdim, M. B., et al. “Brain iron and dopamine receptor function.” Advances in biochemical psychopharmacology 37 (1982): 309-321.
- Erikson, Keith M., et al. “Iron deficiency decreases dopamine D 1 and D 2 receptors in rat brain.” Pharmacology Biochemistry and Behavior 69.3 (2001): 409-418.
- Ashkenazi, Ruth, Dorit Ben-Shachar, and Moussa BH Youdim. “Nutritional iron and dopamine binding sites in the rat brain.” Pharmacology Biochemistry and Behavior 17 (1982): 43-47.
- Konofal, Eric, et al. “Iron deficiency in children with attention-deficit/hyperactivity disorder.” Archives of pediatrics & adolescent medicine 158.12 (2004): 1113-1115.
- Sever, Yonathan, et al. “Iron treatment in children with attention deficit hyperactivity disorder.” Neuropsychobiology 35.4 (1997): 178-180.
- Konofal, Eric, et al. “Effects of iron supplementation on attention deficit hyperactivity disorder in children.” Pediatric neurology 38.1 (2008): 20-26.
- Zylowska, Lidia, et al. “Mindfulness meditation training in adults and adolescents with ADHD: a feasibility study.” Journal of Attention Disorders 11.6 (2008): 737-746.
- Mitchell, John T., et al. “A pilot trial of mindfulness meditation training for ADHD in adulthood: impact on core symptoms, executive functioning, and emotion dysregulation.” Journal of attention disorders (2013): 1087054713513328.
- Grosswald, Sarina J., et al. “Use of the transcendental meditation technique to reduce symptoms of attention deficit hyperactivity disorder (ADHD) by reducing stress and anxiety: an exploratory study.” Current Issues in Education 10 (2008).
- Travis, Frederick, Sarina Grosswald, and William Stixrud. “ADHD, brain functioning, and transcendental meditation practice.” Mind Brain J Psychiatr 2.1 (2011): 73-81.


Was this written in the ’90s? lol. Where’s Piratall? It’s way better than any of these. It’s the only thing I’ve found that works better than Adderall. All the eSports pros take it now too, partly because it doesn’t show up on drug tests, and partly because it just works better than Adderall. One capsule has the same effect as 30mg of Adderall. You guys should really update your guide for the 21st century.
What’s piratall? Oh I just googled it. It’s literally nothing more than huperzine a. All that does is increase choline so I seriously doubt that one capsule has the same effect as 30 mg of adderall. Where did you get these claims from?
>Where did you get these claims from?
From his marketing training materials I bet.
As for the actual article, Cyclazodone and N-Methyl Cyclazodone could somewhat fit the criteria, both being pemoline derivatives. They are considered dopaminergics through an as-of-yet unknown mechanism. Notably, they have little affinity for noradrenergic receptors, unlike current prescription stimulants for ADHD, thus they pose a lesser chance of sympathomimetic side-effects, while also not affecting endogenous intracellular dopamine.
They lean closer to the research chemical end of the spectrum, but based on the information currently available they might be safe (some people are worried about possible hepatotoxicity due to pemoline, the parent compound, being withdrawn from the market because of it but I’ve never seen actual evidence that Cyclazodone would cause it). Unfortunately, there aren’t many studies available, with most of this information being taken from the compounds patents’ documents.